Joe Biden hirosimai látogatása a G7 keretében ismét felszínre hozta annak a birodalomnak a cinikus emlékét, amely 78 évvel ezelőtt „ezer nap” erejét szabadította rá a védtelen lakosságra.
Julius Robert Oppenheimer az új-mexikói sivatagban látta atombombáját felrobbanni. 1945. július 16-a volt, és a Szentháromság-próba volt az imperialista racionalitás végső kifejeződése. A geopolitikai forgatókönyvhöz az atombomba is hozzájárult. „Tudtuk, hogy a világ már nem lesz a régi… egyesek nevettek, voltak, akik sírtak… a legtöbb ember csendben maradt” – emlékezett vissza Oppenheimer, miközben a földre nézett, talán öntudatos szégyenérzettel, mintha bocsánatot kérne a jövő generációitól. Az öröksége az azonnali és hatalmas halál volt.
Ezzel az Egyesült Államok lett a történelem első atomhatalma.
Néhány héttel később, augusztus 9-én ugyanezt a plutónium prototípust, a Fat Man-t ledobta az amerikai Bocks Car bombázó a japán Nagaszaki városára. Ha a hirosimai bomba, amely két nappal korábban megdöbbentette az emberiséget, a civilizációs hanyatlás apoteozisának a megnyilvánulása, Nagaszakié nem talál szavakat, amelyek igazolnák az ilyen fokú atrocitást, egy borzasztó horrort. A japán birodalmi hadsereg Kínában és Indokínában elkövetett egyetlen bűnét sem hajtották végre ezekkel a robbantásokkal, amelyek kétszer is „ezer nap” fényét robbantották rá a polgári lakosságra.
Nyugat-Európa történelmi barbársága elképzelhetetlen volt, de az Egyesült Államok barbársága messze felülmúlta azt.
Az az érv, hogy ezeket a tömegpusztító fegyvereket (WMD) a további halálesetek elkerülésére és a háború befejezésére használták, egyike azon hamisságoknak, amelyekhez az amerikai imperializmus hozzászoktatta a világ déli részén élő népeket.
A tét valójában a geopolitikai fölény volt a második világháború közeli vége után, vagyis maga a kapitalizmus válsága által elindított hegemón átmenet.
Az Egyesült Államok számára a Szovjetunióval való, Japán elleni együttműködés központi problémává vált, amellyel szemben a „túlsúlyos hatalom” üzenetét kellett átadnia.
Egy kapitalista és gyarmati világban annak, aki királlyá akarta koronázni magát, romok és árnyékok hegyén kellett lovagolnia, gyakorolva ezt a hatalmat.
„Nyugat-Európa történelmi barbársága elképzelhetetlen volt, de messze felülmúlta az Egyesült Államok barbársága.”
Az Enola Gay repülőgép tüzére és fotósa a következő szavakkal jellemezte a hirosimai detonációt:
„Elkezdtem számolni a tüzeket. Egy, kettő, három, négy, öt, hat… tizennégy, tizenöt… ez lehetetlen. Túl sok van ahhoz, hogy megszámoljuk. Itt jön a gombaforma, amelyről Parsons kapitány mesélt nekünk. Olyan, mint a bugyborékoló melasz tömege. Terjed a gomba (…) A városnak mindez alatt kell lennie. 70 000 ember halt meg villámgyorsan, árnyékuk az aszfalton maradt. A film- és fényképfelvétel lenyűgözően nagy és néma”.
A cél eléréséhez az erőt fel kell mutatni, látványossá kell tenni.
- augusztus 15-én a legyőzött japán császár elmondja élete első rádióbeszédét:
„Az ellenség egy új és kegyetlenebb bombát kezdett bevetni, amelynek kárt okozó ereje valójában felbecsülhetetlen, és sok ártatlan életet követel. Ha folytatjuk a harcot, az nemcsak a japán nemzet végső összeomlásához és pusztulásához vezetne, hanem az emberi civilizáció teljes kihalásához is.”
Hirohito így fejezte ki Japán teljes megadását. Ez volt az első alkalom, hogy hangját nyilvánosan hallhatták. A kontinens feletti birodalmi terjeszkedés iránti vágya belefulladt a csend és a pusztítás tengerébe, amelyről soha nem gondolta, hogy saját nemzetét érheti. A két robbantásban több mint 250 000 ember halt meg, százezrek pedig vakságot, égési sérüléseket és rákot szenvedtek.
Amikor a B-29-es bombázó bombát dobott Hirosimára, a vadonatúj San Francisco Chartát – amelyből az ENSZ született – alig két hónappal korábban írták alá, hogy „megvédje a békét és az emberi jogokat a világban”. Miután látták ezt a barbárságot, úgy döntöttek, hogy létrehozzák az ENSZ-t. A világ tudatában kialakított koncentrációs táborokkal – amelyek a nácizmus előtt Európában elképzelhetetlenek voltak, de Délen évszázadok óta ismertek – a nyugati hatalmak nemzetközi rendszert hoztak létre az újabb emberi katasztrófák megelőzésére. De Japán nem volt Nyugat, sem Kína, sem Indokína, sem Afrika vagy Ázsia. A Mi Amerikánk sem volt az.
Miután az Egyesült Államokat nukleáris technológiájában 1949-ben a Szovjetunió, 1964-ben pedig Kína utolérte, nem jöhetett volna létre közvetlen háború a két nagy nemzetközi hatalmi tömb között. Ahogy Vijay Prashad kijelenti „Washington Bullets” című könyvében:
„A fő ellentmondás az 1945 utáni években nem Kelet és Nyugat között volt – a hidegháborúban –, hanem Észak és Dél között: imperialista háború a dekolonizáció ellen”.
A háború befejeztével az Egyesült Államok a „szabadság kezesévé”, a világbéke egyedüli őreként lépett elő, és gyorsan szövetkezett régi ellenségeivel – Németországgal és Japánnal –, hogy szembeszálljon régi-új ellenségével: a nemzetközi kommunizmussal. Azt mondják, hogy a koreai háborúban, a Chosin-i csatában elszenvedett vereség után, ahol a kínai néphadsereg támogatása központi szerepet játszott a koreai kommunisták számára,
Douglas MacArthur tábornok 26 atomfegyver küldését kérte a kínaiak megtámadására.
Ennek az országnak nemcsak volt bátorsága új forradalmat kirobbantani, hanem egy testvérnemzet támogatására is a birodalmi hódítások ellen. Harry Truman amerikai elnök határozottan visszautasította.
Ugyanaz az elnök, aki két bombát dobott le, aki elindította a vezetéknevét viselő híres doktrínát, ezúttal nem humanitárius megfontolásból utasította vissza a kérést.
Eközben a tengely ellen harcoló népeknek most az ENSZ-ben megkötött jogok elismeréséért kellett küzdeniük, hogy a népirtások ne ismétlődhessenek meg láthatatlanul az első világon kívül. Az UNHCR szerint a vietnami háború 20 éve alatt 2-6 millió vietnami és közel egymillió amerikai katona – többségük afrikai származású – halt meg. Az imperialista gyarmatosítás nem tekintette méltó riválisának Vietnam népét, hiszen nem is tekintette őket embernek. A jenkik apokalipszist hagytak maguk után, de nem tudtak győztesen trónolni csonthegyükön.
„A háborúnak vége, az Egyesült Államok a „szabadság garanciájaként” jelent meg […], és gyorsan szövetkezett régi ellenségeivel – Németországgal és Japánnal –, hogy szembe szálljon régi-új ellenségével: a nemzetközi kommunizmussal.”
A vietnami tehetetlenségüket bosszúból Afrikában vetették be. Ezen a kontinensen a CIA és bábkormányai igazi sporttá tették a népszerű vezetők meggyilkolását. Patrice Lumumba kongói meggyilkolásától kezdve az UNITA és az FNLA CIA általi támogatásáig és finanszírozásáig Angolában – amely késleltette a függetlenséget, és megtagadta az igazságosság és az egyenlőség jövőjét a szétesett országtól – egy háborúval, amely 800 ezer áldozatot, 4 millió menekültet és mintegy 100 ezer megcsonkítottat hagyott maga után. Évekkel később új fejezetük lesz a kontinens másik oldalán, Szomáliában, amikor „szabadságtól” és „humanitárius segélytől” védve beavatkoztak, hogy garantálják az ország állítólagos olajtartalékait. Szomáliaiak százai haltak meg, akiket helikopterekről lőttek le.
A globális káosz elvetésének nemzetvédelmi stratégiája
A hirosimai és a nagaszaki bombázást követő időkben az Egyesült Államok vezette kapitalizmus a legmodernebb technológia bevezetésével, a gazdasági növekedés és a területi terjeszkedés pillanatát élte meg. Világossá kell tenni, hogy az afrikai bennszülött és latin közösségek hasonló mértékű kizsákmányolást, rasszizmust és elnyomást szenvedek el a birodalmon belül. Szervezeteik és vezetéseik nagy része üldöztetés alatt áll; szelektív merényletekkel, mint például Malcolm X és Martin Luther King ellen, vagy több száz bebörtönzéssel. Jelenleg 200 őslakos közösségből származó ember van az Egyesült Államok börtöneiben; a bebörtönzöttek többsége több mint három évtizede raboskodik.
A Kelet elleni terrorista háborúk
Az első beavatkozás a Perzsa-öbölben Irak ellen 1991-ben történt. Az olaj volt a motiváció az Egyesült Államok imperializmusa megkezdte egyedi világuralmát, néhány hónapon belül több mint 200 000 ember halt meg. De a legszörnyűbb mészárlást nem a hagyományos fegyverek, hanem a gazdasági blokád okozta. Az ENSZ adatai – ami nem túl hasznos a háborúk megelőzésében, de értékes információkat generál azokról – azt mutatják, hogy körülbelül 1,7 millió iraki civil halt meg az Egyesült Államok által bevezetett brutális szankciórendszer következtében Az áldozatok fele gyermek volt.
Az iraki háború – a soha nem létező vegyi fegyverek háborúja – 2003-ban kezdődött, és legalább félmillió-egymillió halottja volt. Nafeez Mosaddeq Ahmed újságíró szerint csak Irak esetében a gazdasági háború 1991 és 2003 között 1,9 millió iraki halálát okozta. 2003-tól pedig még egymillióval kell számolni. Ez összesen körülbelül 3 millió iraki életet jelent. Ha hozzáadjuk az afganisztáni, pakisztáni és iraki halálos áldozatokat, a számok elképesztőek. A Bazz-párti értékeléseit eltekintve világossá vált, hogy az Egyesült Államok sem demokráciát, sem szabadságot, sem emberi jogokat nem hozott ezeknek az országoknak.
Szíriában nem sikerült megváltoztatni a politikai rendszert, de a háború közel 10 éve alatt 384 ezren haltak meg, többségükben civilek, valamint 5,7 millió ember menekült el és több mint hatmillió volt a belső menekült a harcok miatt. Szíriában, ahol egykor a régió egyik legmagasabb életszínvonala volt, a gazdaság és az infrastruktúra összeomlott, az újjáépítés költségeit több mint 400 milliárd dollárra becsülik. A bombázások mellett az imperializmusnak volt egy másik titkos fegyvere is, az ISIS, amely laboratóriumi patriarchális fundamentalizmusát alkalmazta, és amelyet a régió és különösen a kurd közösségi szervezetek elpusztítására importáltak.
Ha átfésülnénk ezt a sokszínű és gazdag teret, ami a Mi Amerikánk, akkor több közös elemet találnánk.
Van azonban egy, ami kiemelkedik: a terror és a kifosztás, amelyet a „világok elpusztítója” generál, az az imperialista barbarizmus, amely a Kubától néhány mérföldnyire fekvő Rio Bravo túloldalán száll síkra, és az emberek ellenállnak az ellenállhatatlannak: több mint 60 éve blokád alatt álló sziget.
Az ENSZ-nek benyújtott legutóbbi jelentés szerint 2019 októberében a blokád közel hat évtizedes alkalmazása során felhalmozott károk elérik a 140 milliárd dollárt. A Kuba elleni terrortámadások újabb fejezetet jelentenek. Becslések szerint legalább 3000 halálesetet okoztak. A terroristák mindig északról érkeztek, vagy ott kerestek menedéket, minden kiváltsággal.
Juan Bosch a birodalom feltételezett fia, a diktátor, Rafael Leonidas Trujillo bukása után lett a Dominikai Köztársaság elnöke. Mivel Bosch professzor szuverén és méltóságteljes politikája nem tetszett az USA oligarcháinak, 1963-ban puccsot hajtottak végre, amikor a Dominikai Forradalmi Párt még egy éve sem volt kormányon. Ám a népszavazás és az alkotmány védelmezői felvették a harcot, és hamarosan visszaszerezték a hatalmat, amikor Lyndon Johnson amerikai elnök, aki meg volt győződve a lojális erők vereségéről, és félt a „második Kuba” megjelenésétől a Karib-térségben, elrendelte, hogy az amerikai fegyveres erők „visszaállítják a rendet”.
- április 28-án elindították az „Operation Power Pack”-et, ami a Trujillo-politika visszatérését jelentette, amely 31 évig vaskézzel uralkodott. Ez a politika több mint 50 000 ember haláláért volt felelős. „Kiemelkedő” eseményei közé tartozik az úgynevezett „petrezselyemmészárlás”, amelyben haitiak ezreit gyilkolták meg. A név annak köszönhető, hogy az elkövetők az „r” betű gyenge kiejtése alapján azonosították a sziget másik felén élőket. Így nyelvi rasszizmusuk lehetővé tette, hogy különbséget tegyenek azok között, akiket bebörtönöznek, és azokat, akik soha többé nem lélegeznek fel.
A MINUSTAH nem volt az első imperialista beavatkozás Haitin, de példaként szolgál a gyarmati-humanitárius diskurzusban alkalmazott elnyomásra. Ha figyelmen kívül hagyjuk a mészárosokat Papa Doc és Baby Doc – akik a CIA közvetlen parancsára és Ronald Reagan jóváhagyásával szétverték a haiti népet – és Jean Bertrand Aristide 2004-es államcsínyét, akkor több mint 10 000 kolera okozta haláleset, amelyet az amerikaiak irányítása alatt beavatkozó nemzetek sokaságának kisebb partnere, Nepál csapatokat hoztak be. Nincsenek pontos adatok a haiti nők elleni nemi erőszakról…
Pop és a piszkos háború Közép-Amerikában
A 80-as évek a popzene-export és a nagyfokú interferencia évei voltak Közép-Amerikában. Ezek voltak a nicaraguai „kontrák” és az el salvadori mészárlások évei, ahol a helyi hadsereg Washington parancsára mintegy 27 dokumentált civil mészárlást generált 1979 és 1985 között. Összességében az el salvadori háború körülbelül 80 000 embert követelt.
Guatemalában még mindig nincs hivatalos adat. A becslések szerint a háború végén 200 000 halott volt, 45 000 eltűnt, és közel 100 000 menekült el; a maja Quiché népének többsége, egy rasszizmus áldozata, amely a birodalmi politika pilléreként szolgál. A nők ellen elkövetett atrocitásokról sem rendelkezünk pontos adatokkal. De tudjuk, hogy sokan a hegyekbe menekültek, vagy meghaltak a harcokban, miközben sokan továbbra is az igazságosságért és az emlékezetpolitikáért küzdenek.
Guatemala 20. századának második fele reményekkel indult, de a United Fruit és a CIA megszakította azt. A Jacobo Árbenz elleni 1954-es államcsíny a puccsok és beavatkozások hosszú és sötét történetének kezdete volt. A panamai El Chorrillo negyed lakói sokat tudnak erről. Ez a külvárosi negyed viselte az 1989-es tengeri invázió súlyát. Egyetlen panamai kormány sem nyújtott be panaszt nemzetközi fórumokon, és egyetlen panamai elnök sem próbált igazságot tenni a halottakért. Még hivatalos adatok sincsenek. Csak egy elnök tette be a lábát El Chorrilloba, és még csak nem is volt panamai. 2015-ben a VII. Amerika csúcstalálkozóra tett utazása során..
A diktatúráktól a „kábítószer elleni háborúig”
Délen megtörtént a polgári-katonai diktatúrákból a piaci és „alacsony intenzitású” demokráciákba való átmenet, Chile kivételével, amelynek elitje lesz a példa a globális hegemón hatalom számára. Augusto Pinochet egy évtizeddel tovább marad hatalmon, mint a legtöbb diktátor, akárcsak Alfredo Stroessner Paraguayban. A katonai vezetést megfogalmazó Kondor-terv mögött olyan gazdasági és geopolitikai projekt állt, amely a térség gazdaságait a neoliberalizmus irányelvei szerint irányította.
Ha Chilében, Argentínában, Paraguayban, Bolíviában, Uruguayban, Brazíliában vagy Peruban gyilkoltak, kínoztak és eltűntek, az a tőke új szakaszát akarta elősegíteni, útközben szinte minden forradalmi folyamatot lerombolva.
Kolumbiának nem volt szüksége államcsínyre, mert a kormányzó civileknek nem kellett alkotmányellenes szempontot bevésniük rezsimjükbe. Kolumbia egy olyan ország, amely tudta, hogyan kell szembe menni, mert míg a 21. század elején a régió az integráció és a népi folyamatok új ciklusába kezdett belépni, a dél-amerikai ország katonai bázisokkal telt meg és alkalmazta a tervet. A kolumbiai „háborút a kábítószer-kereskedelem ellen” vívták, ami nem más, mint a felkelők elleni küzdelem a társadalmi igazságosság jegyében.
„Délen megtörtént a polgári-katonai diktatúrákról a piaci és „alacsony intenzitású” demokráciákra való átmenet, Chile kivételével, amelynek elitje lesz a példa a globális hegemón hatalom számára.
A kábítószer-kereskedelmet nemhogy felszámolták, de megerősítették, sőt Alvaro Uribe kormányával az elnöki posztot is elérte. Ám ennek a háborúnak 8 millió áldozata, 7 millió lakóhely elhagyása és 10 ezer nyomorultja volt 2000 és 2015 között.
Mindezt anélkül, hogy beleszámítanák az ország vidéki részein félkatonai szervezetek által elkövetett merényleteket és mészárlásokat. A kolumbiai uralkodó osztályok még mindig büszkék „hazafias munkájukra”. Az amerikai katonák itt nemcsak „exportálható stratégiai erőforrásaik” védelmét vállalták, hanem a gyerekeket is bántalmazták. Legalább 53 kolumbiai lányt erőszakoltak meg amerikai katonák és vállalkozók, akik rögzítették a visszaéléseket és eladták a videókat. A kolumbiai igazságszolgáltatás nem emelt vádat a tengerészgyalogság ellen, mert az Egyesült Államok katonai bázisainak területén követték el ezeket a nemi erőszakokat.
Ez a tragédia a 21. század első évtizedeinek mexikóihoz hasonlítható.
A „kábítószer-kereskedelem elleni háború” első következtetése az, hogy a valóságban mindig is az emberek elleni háború volt.
Mexikóban az áldozatok száma 250 000 halott, 71 000 eltűnt, és több millió ember kényszerült lakóhelyét elhagyni. Ez a háború egy történelmi kifosztás csúcsa volt, kezdve az ország felének amerikai kisajátításával, egészen az 1994-ben kezdeményezett szabadkereskedelmi megállapodásoktól az új gyarmatosításig.
És a lista a mai napig tart, egyre hosszabb, zordabb lesz. A puccsok és a destabilizációs kísérletek halmozódnak és átfedik egymást: Honduras, Paraguay, Brazília, Bolívia. Senkata, Sacaba mészárlásai, whipálák elégetése. Berta Cáceres, Marielle Franco meggyilkolása. Chilében az elnyomás, a nem látó szemek, a megerőszakolt fiatal nők. Folytatódik a Venezuela elleni háborúban és az egyoldalú kényszerintézkedésekben.
Valójában a modern kalózkodás legutóbbi akcióját a britek hajtották végre, akik ismerik a témát, és milliárdos venezuelai aranytartalékot őriztek.
Középen Elliott Abrams amerikai diplomata tért vissza az elátkozottak sikátorából, hogy tovább támadja a népeket. Azok a mészárlások, amelyekért Közép-Amerikában felelős volt, kiérdemelte a „Venezuela elpusztítója” kitüntetést. Ezt a népet sokszor mészárolták le a múltban, utoljára Caracazo idején. Ebből a parázsból Hugo Chavez emelkedett ki, aki ellen minden lehetséges módszert bevetnének, hogy megdöntsék.
Ez a hosszú folyamat egy egész civilizáció hanyatlását tárja fel, amely emberi lények millióit taszítja a mélységbe, hogy a leggazdagabb 1%-a obszcén luxusban élhessen.
Ezen a bolygón kétezer milliárdos – általában a globális északi fehér férfiak – kétszer annyi vagyonnal rendelkezik, mint 4,6 milliárd ember (a népesség 60%-a). Ugyanakkor 700 millió ember él rendkívüli vagy mérsékelt szegénységben. Ezek egy egypólusú hegemónia meztelen figurái, amelyet két atombombával, több ezer napalmbombával és több száz államcsínnyel köveztek ki. Mert a hatalomnak meg kell mutatkoznia, mint a bombáknak Japánban, vagy mint a gazdagoknak a Forbes magazinban. Ezt is el kell hallgattatni, mint a napsütést, amely árnyékot hagy maga után.
Ugyanazok az árnyékok tartották fenn az amerikai birodalmat.
Azon a júliusi napon az új-mexikói sivatagban új korszak kezdődött a Szentháromság-teszttel. Oppenheimer sötét miszticizmusából értelmezte a Bhagavad Gita mondataival, de Kenneth Bainbridge, az első atombombák egyik tervezője, évekkel később a Harvard Fizikai Tanszékének vezetője volt az, aki felfogta az új imperialista színpad természetét.
A robbanás után Bainbridge Oppenheimerhez fordult, és azt mondta: „Oppy, most már mindannyian kurvaként eladtuk magunkat a sátánnak.”
_________________________________________________________________________________________________________________________________________________________________________________________________________________________________



 Megszokásból és kényelemből fakadóan az amerikai dollárt világpénzként használják a nemzetközi kereskedelem egyensúlyhiányának rendezésére, de a szankciók ráébresztették a világot a dollár használatának kockázataira. Következésképpen a BRICS-országok hirtelen kibővültek, Argentínára, Egyiptomra, Iránra, Szaúd-Arábiára és az Egyesült Arab Emírségekre is kiterjesztették a tagságot. A szervezet ma már lényegében a világ olajtermelésének teljes egészét és a világ GDP-jének 40-45%-át tartalmazza. Az nyilvánvaló, hogy az átrendeződés már megtörtént.
Megszokásból és kényelemből fakadóan az amerikai dollárt világpénzként használják a nemzetközi kereskedelem egyensúlyhiányának rendezésére, de a szankciók ráébresztették a világot a dollár használatának kockázataira. Következésképpen a BRICS-országok hirtelen kibővültek, Argentínára, Egyiptomra, Iránra, Szaúd-Arábiára és az Egyesült Arab Emírségekre is kiterjesztették a tagságot. A szervezet ma már lényegében a világ olajtermelésének teljes egészét és a világ GDP-jének 40-45%-át tartalmazza. Az nyilvánvaló, hogy az átrendeződés már megtörtént.

























 Nekem, a 20 éve megírt Mi volt előbb Isten vagy Ősrobbanás szerzőjének nagy elégtétel a NewScientist vezércikke, melynek címe: A Kezdet vége.
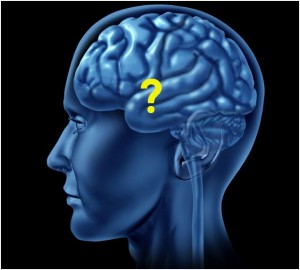
Nekem, a 20 éve megírt Mi volt előbb Isten vagy Ősrobbanás szerzőjének nagy elégtétel a NewScientist vezércikke, melynek címe: A Kezdet vége. 2023 júliusa volt minden idők legmelegebb hónapja, 0,72 °C-kal volt melegebb az 1991-2020 közötti időszak júliusi átlagánál, és 0,33 °C-kal melegebb, mint az előző legmelegebb hónap, vagyis 2019 júliusa.
2023 júliusa volt minden idők legmelegebb hónapja, 0,72 °C-kal volt melegebb az 1991-2020 közötti időszak júliusi átlagánál, és 0,33 °C-kal melegebb, mint az előző legmelegebb hónap, vagyis 2019 júliusa. Hogy a nők első számú kötelességnek érzik, hogy a férfiak figyelmét felkeltsék, az nem egy új megállapítás. Nem is lehet, mert már majom korunkban is így volt. Végül is, ameddig a történelemkönyvek vissza tudnak menni, a nők mindig is meg akar termékenyülni és ehhez iparkodtak kiválogatni a megfelelő férfit, elvégre a művelethez férfire feltétlenül szükség van. És persze a sok gyakorlásnak meg is volt a gyümölcse. A nők ezer módon tudják felhívni magukra a figyelmet. Ennek a figyelemfelkeltésnek azonban mindig is megvolt az érvényes divatja, stílusa és rítusa, amit a nőknek illet betartani. Ehhez a le nem jegyzett szabályokhoz minden generációs és az összes kultúra hozzáadott valamit, így aztán mára szinte művészi szintet ér el a nő-férfi kapcsolatteremtése, legfeljebb nem tudatosodik bennünk.
Hogy a nők első számú kötelességnek érzik, hogy a férfiak figyelmét felkeltsék, az nem egy új megállapítás. Nem is lehet, mert már majom korunkban is így volt. Végül is, ameddig a történelemkönyvek vissza tudnak menni, a nők mindig is meg akar termékenyülni és ehhez iparkodtak kiválogatni a megfelelő férfit, elvégre a művelethez férfire feltétlenül szükség van. És persze a sok gyakorlásnak meg is volt a gyümölcse. A nők ezer módon tudják felhívni magukra a figyelmet. Ennek a figyelemfelkeltésnek azonban mindig is megvolt az érvényes divatja, stílusa és rítusa, amit a nőknek illet betartani. Ehhez a le nem jegyzett szabályokhoz minden generációs és az összes kultúra hozzáadott valamit, így aztán mára szinte művészi szintet ér el a nő-férfi kapcsolatteremtése, legfeljebb nem tudatosodik bennünk.